Teaching a technique to improve health in Haiti

Dr Pollock (2nd from left) provides instruction during a surgical training mission to Rwanda. This year he will take part in a similar mission to Haiti.
Haiti has faced immense challenges since January 2010 when the impoverished nation was shattered by a magnitude 7.0 earthquake that led to over 100 000 deaths. After the quake struck, many Haitians lived in tents for years before being moved to cinderblock shantytowns barely better than the sweltering tent cities. At the same time, the country has been hit by outbreaks of cholera and tuberculosis, and today has one of the highest rates of HIV/AIDS in the Caribbean.
Haiti's first lady, Sophia Martelly, has made the fight against HIV a priority, and the mission I'm now preparing for was initiated when she contacted Dr Jeffrey Klausner, a professor of medicine and public health at UCLA, and asked him to find an expert willing to train surgeons to carry out quick, safe, and painless infant circumcisions.
By reducing rates of urinary tract infection, STIs, cancer, and HIV, infant circumcision can save thousands of lives--something recognized by the consensus statement from the American Academy of Pediatrics released in late 2012, which declared that "the medical benefits of infant circumcision outweigh the risks," and changed the way many in the medical community view the procedure.
When Dr Klausner asked me to contribute my time and skills, and to help raise the money needed to set up the program, he noted that "While $25 000 might not seem like an insurmountable sum for acquiring the instruments, supplies, and infrastructure required to teach a lifesaving procedure, it is a fortune in a country where people live on $1 or $2 a day." Just 72 hours after contacting 50 friends and family members about the mission, I had the money needed--proof that many people care about the desperate situation in Haiti, and a wonderful start to a sustainable public health initiative.
Despite the challenges ahead, my experience performing thousands of circumcisions in Canada, Turkey, China, and a number of African countries makes me optimistic that the mission can contribute to better health outcomes in Haiti. I expect my experience in Rwanda will be especially relevant, since the countries are alike in having trauma-filled pasts.
In 2008, Dr David Patrick, head of the BC Centre for Disease Control at the time, contacted me about visiting Rwanda--a country scarred by the genocidal slaughter of thousands in 1994--where infants were being circumcised using scissors, sutures, and no anesthetic. Knowing that I had developed a 30-second virtually painless surgical technique that would be accepted by Rwandans, Dr Patrick asked me to share my knowledge of this procedure. Today I am still in contact with the surgeons I trained in Rwanda, and they tell me they are using the technique safely and effectively throughout the country.
My mission to Haiti, like my mission to Rwanda, will include a multiday surgical schedule. My colleague Dr Pierre Crouse of Calgary and I will train two physicians using models to demonstrate the technique Iíve developed over the past 20 years, which employs surgical efficiency and extensive pain control, and achieves excellent cosmetic results. The trainee surgeons will practise on the models, assist me with scheduled surgeries, and eventually carry out procedures under my supervision.
By the end of the mission we will have treated more than 200 infants, and the newly trained surgeons will be ready to train others. And everyone involved, including my generous friends and family, will feel blessed to have been part of a program that can be shared with other countries in the Caribbean and duplicated throughout the region.

Dr Pollock holds patient postcircumcision with nurses looking on.

A family with baby just returned to them postcircumcision surgery.
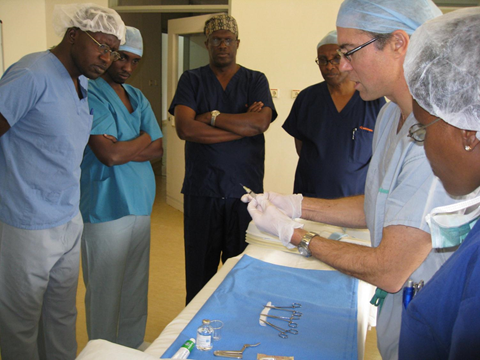
Dr Pollock conducting a teaching session for surgeons from various regions of Rwanda.
hidden
Dr Pollock is a physician based in Vancouver who limits his practice to two office-based procedures--circumcision (all ages) and no-scalpel, no-needle, open-ended vasectomy. Dr Pollock has safely performed 55 000 surgeries over the last 15 years.
