Special feature: Mitufala dokta lanem planti long Vanuatu! (We two doctors learned a lot in Vanuatu!)
“If your hospital is at sea level on the equator, expect to operate at 30°C in 95% humidity, your clothes wet, and everything which can go rusty or moldy doing so. Only insects enjoy such conditions, and you will find plenty of them.”

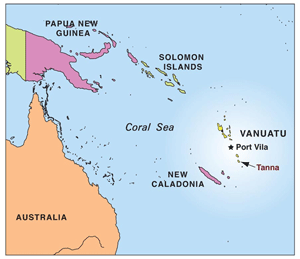
After our first day as the only doctors on the South Pacific island of Tanna, Vanuatu, my wife and I found the quotation above to be quite an accurate description. It is a quote from the introduction to Primary Surgery, an excellent manual of surgical procedures written for general practitioners in developing countries. We found this book in the doctor’s house on Tanna and it was indispensable.
Our adventure began when we arrived at Tanna’s little airport on a hot and humid morning last January. We were met there by the outgoing doctor’s wife and five children. The doctor we were replacing had to take one of his children to Brisbane for emergency medical care, so unfortunately he could not orient us to the island as planned.
We loaded the doctor’s truck with luggage and children and drove the dirt road to Lenakel. At the doctor’s house beside Lenakel Hospital, we dropped the luggage and had a bite to eat. Rather than go straight to the hospital to introduce ourselves, we decided to first go for a cooling dip in Lenakel Harbor.
The ocean was truly refreshing. We swam in the clear blue water over beautiful coral while the children had great fun showing us how they could dive off the reef. Just when we were getting out of the water, we heard a siren. An ambulance stopped at the beach and a nurse stepped out. She told us she had been driving around for the last hour looking for the new doctors. She asked us to come to the hospital right away to see a woman with a postpartum hemorrhage.
My wife Lisa, still in her wet swimsuit, jumped into the ambulance for the ride up to the hospital, and I joined her a short time later.
We saw the patient in the tiny hospital delivery room. The multiparous woman had delivered a stillborn hydrocephalic infant in a remote village then bled for several hours before arriving at the hospital. The midwife had already started two IVs, given oxytocin and ergotomine, packed the vagina, and called the laboratory technician to crossmatch blood.
Sweating profusely, we took her to the operating room. A gecko jumped off the anesthetic machine and scampered across the OR floor. A nurse administered oxygen, ketamine, and valium while we examined the patient. Lisa found only a few remnants of placenta in the uterus, but bleeding continued.
All we could do was pack the uterus, give oxytocin and all seven units of the blood donated by relatives and hospital staff. Fortunately, the bleeding slowed and we were able to fly the woman to Port Vila, the capital of Vanuatu, the following day, where she did well.
Such was our crash introduction to Lenakel Hospital and its staff. They were happy to see us and we were impressed with their friendliness, competence, and teamwork. This held true throughout our 6-month service despite the often trying conditions predicted in the Primary Surgery book.
On Tanna these conditions included not only the heat, humidity, and insects, but the volcanic ash, tropical storms, intermittent medicine and oxygen shortages, equipment malfunction, staff absenteeism, and power and water outages.
So how did two Canadian family doctors come to be living and working in Vanuatu? My wife and I had both started our careers in rural Canada but for the past 10 years have had typical urban general practices in Victoria. We were starting to feel a bit stifled by the narrow scope of our office routine and felt the time was ripe to try something quite different—and far away!
Physicians and their families living on southern Vancouver Island have a unique opportunity to participate in the ViVa Project (Victoria-Vanuatu Physician Project). This grassroots nonprofit society was established 17 years ago by a small group of Victoria doctors in partnership with the Vanuatu government to fill the position of the only doctor on the island of Tanna.
ViVa meets regularly, raises funds to maintain the comfortable three-bedroom doctor’s house and four-wheel drive truck, and organizes the training and replacement of the Tanna physician every 6 months.
We were selected to serve in Vanuatu by a ViVa selection committee and then had to apply and be approved by the Vanuatu government medical licensing board. We prepared for our adventure by first trying to find two locums to cover our Victoria family practices (a separate story in itself, filled with frustration, of which all physicians are familiar!).
Next, we attended the monthly ViVa meetings and orientation sessions to learn from the experiences of others who had gone before us. Several Victoria obstetricians were very helpful in teaching us to do cesarean sections. We spent some time with ultrasonographers and TB clinic doctors, and studied some tropical medicine. Previous ViVa doctors gave us tutorials in Bislama, a form of pidgin English which is one of Vanuatu’s official languages.
Typical of all ViVa volunteers, our total time commitment to the project will exceed 2 years. This includes our attendance at ViVa meetings 1 year before departure, our 6-month service on Tanna, and now a term as ViVa president to foster the recruitment and training of subsequent physicians. The secret of ViVa’s organizational longevity, therefore, is not just the doctor’s unique and enriching third-world experience, but also the doctor’s service to the project before and after.
Tanna is a small island about 30 km 3 60 km with an active volcano. It is extremely fertile in every sense. A huge variety of vegetables and fruit grow year-round. Horses, cattle, goats, pigs, and chickens thrive. The reefs and ocean abound with fish and the population of 30000 grows at a rate of about three new pikininis per day. Its economy is mostly subsistence with some cash provided by coffee exports and tourism.
The Melanesian people who settled in Vanuatu a few thousand years ago were said to be fierce, independent, and cannibalistic. They ate their enemies, including some of the missionaries who bravely ventured onto their beaches in the 1800s. Finally, after years of joint British and French rule as the New Hebrides, Vanuatu became independent in 1980.
It is still a patriarchal society, ruled by tribal chiefs, and is very family and village oriented. On Tanna these days, visitors are greeted with smiles and waves. The closest they will get to being cooked on a fire is to stand on the rim of Mt. Yasur looking into its red hot caldera while dodging flying magma.
Primary health care is delivered from the 40-bed Lenakel Hospital and a dozen village nursing outposts (called dispensaries). The government provides a basic but surprisingly comprehensive drug formulary free of charge for all citizens. The hospital has a functioning operating theatre, X-ray machine, and a laboratory that can do basic hematology and chemistry, gram stains, AFB, and malaria smears, but no other microbiology or tissue pathology.
Lenakel Hospital’s busy outpatient clinic is run by nurse practitioners, and the labor-delivery service is run by nurses and midwives. The doctor attends the inpatients, does consultations for outpatients and complicated obstetrics, performs minor surgery and cesarian sections, and regularly visits the island dispensaries.
We found that the doctor’s life on Tanna is a two-person job. The clinical work easily kept one of us occupied full time (with some reasonable breaks and time off) but the domestic work is also a full-time job. Because we both wanted to practise medicine, we divided the work by switching our medical and domestic roles every other day.
Our children are grown and out of school and came down to visit us, but many doctors have brought their young families who thrive, learn many new things, make new friends, contribute to the community, and have a safe, wonderful, life-changing experience. A variety of home-learning programs are available to bridge the children’s brief school interruption.
The clinical work is fascinating. On the wards, we saw malaria, dengue, typhoid, TB, abscesses, pneumonia, meningitis, and asthma. In the operating room we would do emergency C-sections, vasectomies, tubal ligations, and incision and drainage of abscesses.
Traditional or kastam medicine is practised by most of the population, but there is increasing acceptance of modern medicine, especially surgery and antibiotics. Village bonesetters treat most of the fractures.
One particular patient we saw illustrates both the synergy and conflict that exists with the two views of health in Vanuatu. A young man who lives on a small island near Tanna was playing soccer when he collided with another player and sustained a mid-shaft fracture of his tibia and fibula.
He sought treatment from the traditional bonesetter who, in typical fashion, made three deep kastam cuts over the fracture site, dressed the wounds with leaves, and splinted the leg with bamboo sticks. The patient bled heavily. His family, recognizing that this was life threatening and that modern medicine could help, loaded him into a small boat. After 3 hours on the open sea, he landed on the east coast of Tanna, then traveled another 2 hours on the bumpy road to Lenakel Hospital.
The young man arrived at midnight with his entourage of relatives. He was in a state of shock, delirium, and incontinence from both ends. My wife had the pleasant job of resuscitating him. The next morning, he was alert and feeling much better. His family huddled around as we showed him the X-ray.
We discussed the usual treatment: closed reduction with prolonged immobilization or referral to Port Vila for possible open reduction. This young man didn’t like either option. He and his family wanted a second opinion—from another bonesetter! Despite our caution that he would likely never play soccer again if he did so, he decided to leave, his family carrying him out of the hospital.
Most Vanuatu (ni-Van) patients were very appreciative of the care they received and compliant with their medication. We were repeatedly amazed at the capacity of the human body to heal itself and at the remarkable ability of the ni-Van people to cope with severe illness, pain, and even death.
With the help of antibiotics, we saw many infants, children, and adults recover fully from meningitis, complicated pneumonia, and typhoid fever despite presenting in the very late stages of disease. We were equally impressed to see a variety of seemingly impossible labor presentations successfully deliver vaginally or surgically with mothers and babes making a full recovery.
Over 6 months, we encountered many new and different things in Tanna’s climate, culture, and illnesses, but one constant was the friendliness of the ni-Van people and their appreciation for our small contribution.
We highly recommend this sort of experience to any general practitioner looking for a change. It is a unique learning and teaching opportunity. It is exciting, challenging, frustrating, and sometimes sad, but also exhilarating, joyful, and ultimately fulfilling. You and your family will certainly live a simpler life, do more with less, and face the world with new appreciation and confidence.
The editors of Primary Surgery describe the intrepid third-world general practitioner in these lofty words: “You are an all-rounder, and have one of the last remaining opportunities to practise the totality of medicine, rather than some infinitesimal corner of it. Sub specie aeternitatis, in the mirror of eternity, you are a hero and will surely be recognized and remembered as such.”
Suggested reading
Primary Surgery. Vol 1. Ed M. King, P. Bewes, J. Cairns, et al. Oxford: Oxford University Press, Kenya Ministry of Health, German Federal Ministry for Economic Cooperation; 1990.
hidden
Dr Leduc is a GP with a practice in Victoria, BC, and a member of the Victoria-Site Faculty for the UBC Family Practice Residency Program. His wife, Dr Lisa Veres, is also a GP in Victoria. More information on the Victoria-Vanuatu Physician Project can be found at www.ViVaProject.ca.
