Parallel worlds: Reflections from Centro de Salud Santa Clotilde, Peru
Daily experiences in the Peruvian Amazon during a rural family-medicine elective.
Daily experiences in the Peruvian Amazon during a rural family-medicine elective.
Things are not always what they seem. This summarizes my daily experiences in the Peruvian Amazon for a rural family-medicine elective. Although on first sight the situations and approaches used seemed drastically different from what would be the norm in Canada, I quickly realized that they were just alternative paths to the same endpoint in most cases, and there were more similarities in play than differences.
The Centro de Salud Santa Clotilde (CSSC) is located adjacent to the Rio Napo, 5 hours upriver by boat from Iquitos in northeastern Peru. The CSSC provides health care and support services to approximately 15 000 predominantly Indigenous people spread throughout roughly 100 villages. The Missionary Sisters of Our Lady of the Angels from Quebec took on the tasks of education and health care in the region between 1951 and 1991 as nurse-nuns. Beginning in the mid-1980s the physician-priests, Padres Jack McCarthy, MD, and Maurice Schroeder, MD, began to provide medical services and transformed the facility into its current state.
The centre now boasts a 30-bed inpatient ward, simple OR, birthing room, emergency-procedures room, laboratory, and pharmacy. Inpatient, outpatient, emergency, obstetrical, pediatric, psychological, and dentistry services are offered. Although the infrastructure is basic, the hospital staff and the services they provide are certainly not. During my time at the CSSC I came to appreciate the breadth of knowledge and amount of advocacy that permeated the daily work at the hospital.[1]
Interdisciplinary teamwork
Each day began at 6:00 a.m. with the town’s public-radio tower crackling to life with the Peruvian national anthem, followed by town news. Hospital rounds started promptly at 7:00 a.m. and took the form of a group meeting where announcements were made and everyone had a chance to speak. Everyone, including at times our resident dogs and chickens, then rounded on the inpatients, thus ensuring all team members were involved in each individual’s care and informed of disposition plans. I found it to be an inclusive environment with time to learn and discuss all aspects of care as well as interact with all teams, something which is often lost in large centres in the first world due to high patient volumes. This casual communication continued throughout the day with various team members often dropping by to ask for clarification or to share important details.
The casual, open environment continued in the outpatient clinic, which is where the majority of working hours were spent. Whenever there was confusion about a case, an interesting teaching point to be made, or a second opinion was required, it was a simple exercise to walk to a nearby office and make inquiries. The physicians provided abundant information on diseases I had never encountered in the flesh, such as malaria, leishmaniasis, leptospirosis, and ascariasis. They were also an incredible resource on critiquing physical examination skills, refining questions on history, and expanding my knowledge of common ailments such as arthritis, respiratory infections, and traumas.
Although resources were scarce, there was access to current evidence-based medicine, and I consistently saw the Peruvian doctors using evidence-based applications or quickly researching diagnostics or treatments via our intermittent satellite Internet connection. However, due to the demands of a low-resource hospital attempting to adequately service so many, there was little time for scholarly endeavors. The demands led to a number of stressful moments, but also added to the camaraderie that came as a result.
During my first few dizzying days in this new environment I tried to get a handle on hospital protocols and village culture. It was comforting to see my old friend the SOAP note when I flipped open my first handwritten foolscap chart, but then I realized that I didn’t know what a gota gruesa or a heces fecales was (later determined to be a malaria smear and fecal smear), nor did I understand the various shorthand notes and synonyms for Spanish descriptions. These would soon become second nature and comparable to vital signs to me. Although I had spent numerous years studying and practising Spanish in Canada and abroad, I found learning the Spanish medical terminology a steep transition. To add to the confusion, during the first few afternoons I found myself standing alone in the previously bustling clinic without electricity. This was later explained by the town’s afternoon siesta and the public generator, which was only operational for select hours in the morning and evening (exceptions to this rule, however, included village celebrations, where one was serenaded until the early hours of the morning with the latest Latin rhythms). As I adapted to the differences in protocol, paperwork, diagnostics, diseases, and lifestyle, I realized that the basic foundation of care and clinical reasoning remained the same, and I fell into a rhythm.
Patient expectations
Communication between doctors and patients was another learning curve. The relationship was more formal than in Canada. Although physicians would have likely happily included patients in the decision-making process—something we strive for in Canada—patients seemed more comfortable simply taking direction. This may have had some roots in the poverty and lack of education that many patients struggled with, which became apparent to me when I learned that the government-assisted health insurance that the majority of patients accessed was reserved for the poorest in the nation. This scenario wasn’t always the case, however, as some patients requested scarce medications and physicians had to navigate difficult conversations, just as they do in Canada.
Scarce resources
Although the physicians possessed a wealth of knowledge and gave extraordinary care given the resources available, there were shortcomings with technology, medications, general supplies, and access to specialists. Almost daily, the pharmacists would announce that the hospital had run out of paracetamol or ampicillin and that we would not be getting a shipment for a month or two. It was also a privilege to have electricity at times when it was most needed, such as during procedures and deliveries, so you could turn your headlamp off for a moment. As well, because we were not equipped to perform any type of imaging other than simple ultrasounds, everyone played it safe with patients and had a low threshold to admit-and-watch or transfer if they worsened. To complicate matters further, disposition was a unique challenge given the location and environment. Determining where and when patients could safely go home became as important as their diagnosis.
Transferring a patient to a specialist had its challenges as well. The Peruvian doctors told me that Iquitos had its limitations and some physicians there were reluctant to accept certain transfers. Though this appeared to be specialist-dependent, it was disheartening when encountering patients adversely affected by cataracts or pterygium, and showed that the people in the Napo region had to contend with more than poverty and a lack of resources. In addition, some patients were unable to afford the journey and thus were powerless to receive further treatment.
Similarities rather than differences
Canada and rural Peru contrast significantly in areas such as disease type, access to care and medicines, technology, and specialist services. However, I also spent time in Inuvik and Tuktoyaktuk, NWT, along with areas of rural BC, and noticed the same lack of opportunity, poverty, and diseases such as tuberculosis present.
This is illustrated by Canada having one of the worst infant mortality rates according to the Organisation for Economic Cooperation and Development.[2] During my time in Peru many of the tenets of the Canada Health Act came to mind, along with why they exist—universality, accessibility, and comprehensiveness.[3] The provisions of the Act ensure that all Canadians have access to timely advanced care, which is not the case in rural Peru, and may be a reason why Peruvians struggle with diseases that are routinely managed in Canada, such as diabetes, hypertension, and their sequelae.
And the comparisons are not limited to rural populations; the people in the Napo region struggle with the same issues of alcohol and drug misuse, domestic violence, and mental illness that plague our urban cores in Canada—which I saw during my clerkship training at St. Paul’s Hospital in Vancouver. I’m thankful for my time spent in both places. It has made me realize that poverty has the same face no matter what the climate or ethnicity.
Patient education
It would be naive to think that I could make recommendations on how to better deliver care to rural Peruvians having spent 1 month in a single location. However, given that many of the causes of inadequate care appear to find roots in poverty—a theme that translates across many countries, and one I’m struggling to fully understand—some simple reflections can be made.
Although funds are limited in any country, a greater portion dedicated to health care is always helpful. Also, alleviating the stressors on the determinants of health, such as poverty and a lack of formal education and employment opportunities in underserved regions, would be of benefit.
One area that doesn’t carry a large price tag but has a potentially large impact is patient education. Although the physicians attempted to educate patients and their families on disease processes and medications daily, it often seemed to fall on deaf ears. I encountered daily conversations about the implications of sporadic use of antimalarials and antibiotics, reluctance to use the vaccinations that were available, and the importance of not sharing medications. It’s possible that certain misconceptions are rooted in the lack of formalized education as well; however, educating patients on appropriate medication use, such as when presented with patients taking both ranitidine and omeprazole for osteoarthritis, seems correctable regardless of educational level. Again, these experiences echo similar conversations occurring in clinics and hospitals throughout Canada.
A privilege to learn
I’m deeply grateful for the privilege to have worked with and been mentored by the great physicians and staff at the CSSC. I encountered diseases that I wouldn’t have seen in Canada, which is of great importance given our large immigrant population and Canadians’ frequency of travel. I will be a better physician having learned to manage various exotic diseases and refined certain basic skills in a low-resource area. There were drawbacks—dealing with frequent power outages, eating a daily diet of eggs, and being covered in ants and kept up at night by neighborhood dogs (that rested all day). But the experience had benefits that I couldn’t recreate, and there are many moments that will be hard to forget—interviewing and assessing patients by headlamp with donated equipment during rainstorms, or watching cockroaches scurry out of my underwear while I searched my shelf for the reprieve of clean laundry.
It was humbling to be immersed in a different culture, language, and health care system, and I leave Santa Clotilde with much empathy for the immigrants and travelers who are attempting to navigate the Canadian health care system. And I will most definitely take time to listen and understand patients and their families, even when communication is challenging and it’s easy to give up, because if you stay a moment longer you’ll realize that most people are searching for the same things.
Acknowledgments
I would like to extend my sincere gratitude to the entire staff at the CSSC for allowing me the privilege to take part in such a noble and enriching effort.
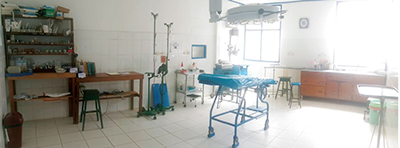 |
| In addition to the simple opertating room shown here, the facility has a 30-bed inpatient ward, a birthing room, a lab, and a pharmacy. |
 |
| View of the hospital courtyard with inpatient ward to the right and outpatient services to the left. |
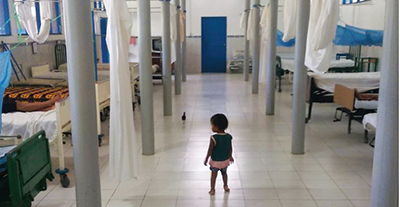 |
| A child follws a chicken through the inpatient ward. |
hidden
This article has been peer reviewed.
References
1. PANGO Canada. Accessed 21 August 2017. www.pangocanada.ca.
2. OECD Data. Infant mortality rates. Accessed 11 November 2017. https://data.oecd.org/healthstat/infant-mortality-rates.htm.
3. Justice Laws Website. Canada Health Act. Accessed 11 November 2017. http://laws-lois.justice.gc.ca/eng/acts/C-6.
hidden
Mr Burton is a fourth-year medical student at the University of British Columbia in the Vancouver-Fraser medical program. Mr Burton’s interests include primary care and emergency medicine.

