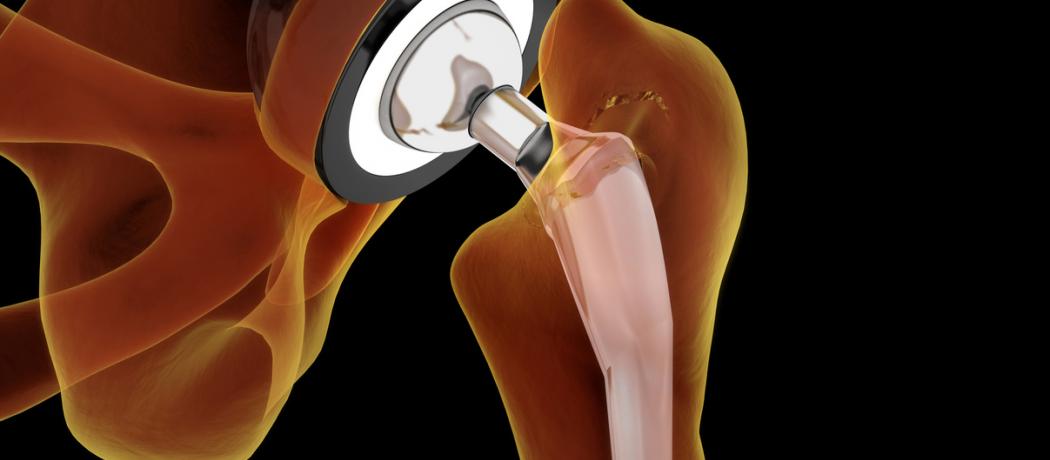
On 28 August 2019 I had a total replacement of my left osteoarthritic hip. With spinal anesthetic I was more or less awake during the procedure to hear the buzz of the saw and the blows of the hammer as my prosthesis was being inserted. I was awake enough to reflect that my maternal grandfather, Dr Bertholm Widder (1873–1910), was in training for orthopaedic surgery at the Berlin hospital where Professor Themistocles Gluck attempted the first hip replacement operation in 1891. The patient’s hip joint was destroyed by tuberculosis. Gluck replaced the femoral head with ivory, using nickel-plated screws, plaster of paris, and pumice with resin.
In 1925, American surgeon Dr Marius N. Smith-Petersen created a glass mold that fit over the femoral head. When the glass shattered, Smith-Petersen and Philip Wiles moved on to using stainless steel bolts and screws.
In 1953 English surgeon Dr George McKee began using metal on metal prosthesis with good results, but Sir John Charnley is considered the father of the modern total hip replacement with his low-friction arthroplasty introduced in 1960.
Although during my recent saga my immediate focus was on the surgical procedure, I was most impressed with the health-team approach to overall patient care, from my diagnosis to well after my discharge from the hospital, and even ongoing now, involving nurse, physio, and occupational therapy educators and practitioners. Through preoperative lecture presentations, demonstrations, and practise opportunities they provided for all the required home and personal preparations. The hospital had seamless scheduling procedures for pre-operation meetings with nurse clinicians, anesthetists, and the required cardiology and other departments’ services during the expected short hospital stay. Just a few hours after my operation I was walking (cautiously!) with a walker in the hospital corridor. Expert nursing and additional physio and occupational therapy services made sure that all home equipment was in place for my recovery period.
In the 1960s I worked under the direction of Dr Jack McCreary, then Dean of Medicine at UBC, on the health team concept, but even we did not conceptualize quite what has developed in this area in the last few years. In the context of the Vancouver Coastal Health region, once the referral process begins with the family physician, a patient-focused, highly organized chain of events unfolds. I felt surrounded by a multitude of professionals and administrative staff who with their expertise in their various fields and with clock-like precision attended to my needs. Health teams in action. I am most impressed and thankful.
—George Szasz, CM, MD
This posting has not been peer reviewed by the BCMJ Editorial Board.